What is Ozempic Face and What Can You do About It?
By Elena Allbritton, MD
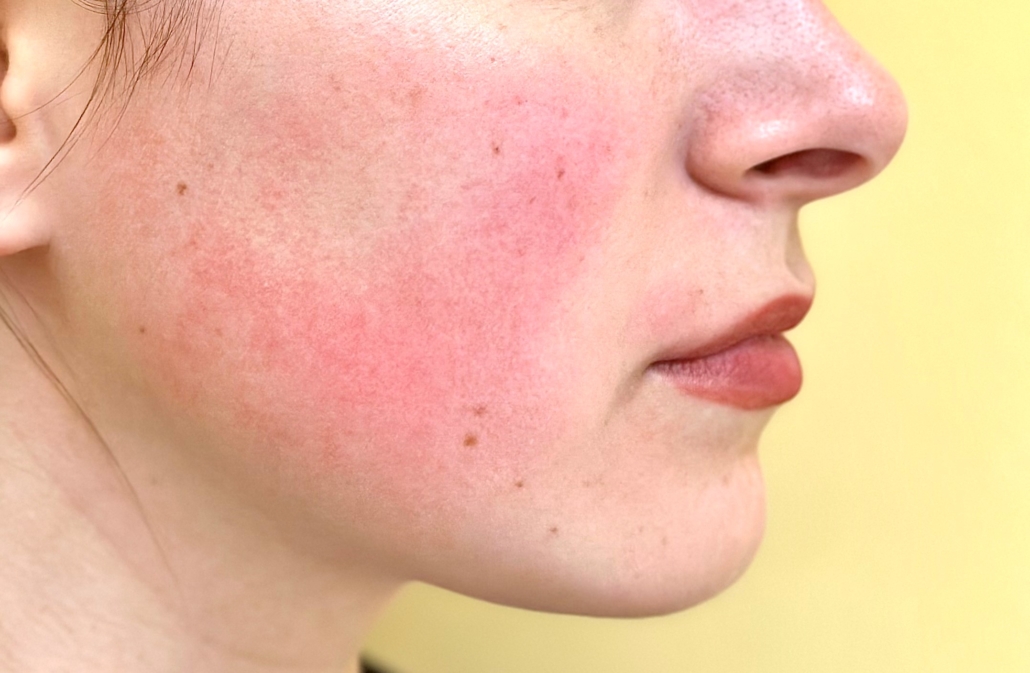
With over 2.3 million views of #ozempicface on TikTok and social media abuzz with stories about “Ozempic face,” numerous articles have been written about the facial changes following rapid and substantial weight loss. The phrase was coined by NY dermatologist Dr. Paul Frank, who observed his patients on weight-loss medications complaining about their gaunt, sagging faces. Although linked with Ozempic, a prescription drug developed to treat diabetes, the real culprit behind “Ozempic Face” is significant weight loss. So is the trade-off for dramatic weight loss a wrinkled, older-appearing face? The short answer is yes, although some people are more susceptible than others.
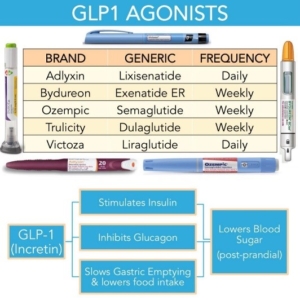
Source: GrepMed
At almost $90 Billion, the U.S. Weight Loss Industry has reached a historic peak. The rise of prescription drugs such as GLP-1 agonists (Ozempic, Wegovy, Rybelsus, Trulicity, Victoza, and Saxenda; semaglutide, dulaglutide, liraglutide) and combination GIP/GLP-1 agonists (Mounjaro and Zepbound; tirzepatide) has significantly affected the diet industry and revolutionized the treatment of obesity and diabetes. Estimates are that one in eight adults has tried one of these medications for weight loss or to manage diabetes.
How do Ozempic and Simular Drugs Work?
Originally designed as a treatment for diabetes, Ozempic works by mimicking the action of the GLP-1 (glucagon-like peptide-1) hormone, which regulates blood sugar levels and slows down digestion, leading to reduced appetite and, ultimately, weight loss. GLP-1 (incretin hormone) is produced by the gut and increases insulin production from the pancreas only when blood sugar levels are elevated. This targeted action reduces the risk of hypoglycemia (low blood sugar), which is a common concern with other diabetes medications
Ozempic is one of several drugs that have gained immense popularity for their off-label use in weight loss. Weight loss from these drugs is significant and can be up to 15-25% of body weight over the course of 1 – 1.5 years.
- FDA approved for treating diabetes: Ozempic, Trulicity, and Mounjaro (administered by injection weekly or daily (Victoza).
- Rybelsus is an oral semaglutide GLP-1 agonist taken daily for diabetes management.
- FDA approved for weight loss: Wegovy (weekly injection semaglutide) and Saxenda (daily injection liraglutide) are the only GLP-1 medications FDA approved for weight loss. Zepbound (weekly injection tirzepatide) GIP/GLP-1 agonist
** Weight management for obesity (body mass index [BMI] ≥ 30) or overweight (BMI ≥ 27) plus at least one weight-related comorbidity such as hypertension, type 2 diabetes, and high cholesterol.
“Ozempic Face” = Rapid Weight Loss Face
When fat loss occurs in the body, it occurs throughout the body and not in a specific area. This effect is not unique to Ozempic and can be seen with any significant weight loss, especially if it happens quickly. However, because Ozempic is so effective, the facial changes can be more pronounced and have led to the moniker “Ozempic face.” Facial fat changes are more noticeable once patients lose 25 to 30 pounds, but it varies based on the starting weight, height, and facial fat composition.
Fat pads in the face provide structure and volume to the face. Loss of the “youthful” fat creates hollowness around the eyes, cheeks, and temples. This skeletal and aged appearance occurs with normal aging as well. Other factors that increase the chances of developing these facial changes include older age (more common in middle-aged patients and older) and patients with less skin elasticity because of lifestyle (sun damage, smoking), genetics, or skin type. Fair-skinned patients tend to have thinner, less elastic skin and are more susceptible to showing signs of “Ozempic face.”
Can You Treat “Ozempic Face” or Reduce the Risk of It?
To manage the skin and facial changes that occur while taking Ozempic and other weight loss drugs, it is important to see your dermatologist or provider for soft tissue fillers. The ideal time to address facial volume loss is when the patient has achieved their weight loss target. Gradual tapering of weight loss medications can help avoid rebound weight gain once patients stop their medications.
- Dermal fillers replace the volume loss and can create a fuller, more youthful face. There are several FDA-approved forms of fillers that can be injected into areas such as the cheeks, chin, temples, and under eye area. Seeing a licensed, experienced provider can reduce the risks from dermal fillers which include pain, tenderness, swelling, infection, migration of filler, and more significant complications such as vascular occlusion and tissue necrosis. To replace global facial volume loss, it can take a significant amount of filler. In addition to Hyaluronic Acid fillers (Restalyne, Juvederm), biostimulatory fillers such as poly-L-lactic acid (Sculptra) lead to prolonged effects from collagen production.
- Skin hydration with medical-grade skin care can promote collagen production, improve skin elasticity, and reduce the appearance of wrinkles. Moisturizers with hyaluronic acid and retinoids can improve skin hydration and texture. Consider estrogen supplements for post-menopausal patients to decrease wrinkles and sagging skin.
- Autologous fat grafting is a longer-term option that may be performed under location anesthesia.
- Energy-based skin tightening treatments such as Radiofrequency microneedling, Ulthera, or Softwave are typically beneficial in younger patients with better skin elasticity.
- Surgical treatment (browlift, blepharoplasty, partial or full facelift, and neck lift) may be needed to address loose skin in older patients or those with more significant facial sagging/aging.
- Decrease risk of “Ozempic Face” by aiming for gradual weight loss (1-2 pounds per week) which gives the skin more time to adjust to changes. Work with your provider to ensure adequate nutrition – supplement with a multivitamin containing iron and Vitamin D and increase protein content to slow lean body mass loss and reduce the risk of hair loss due to telogen effluvium (hair shedding). Titrate the dose of the medication monthly or as needed. Fullness is felt almost immediately on GLP-1 agonists and most patients report decreased cravings. Increase strength training to maintain basal metabolic rate and lean body mass while on medication.
Conclusion
Obesity treatment and weight loss management are increasingly important today. New medications such as GLP-1 agonists and combination GIP/GLP-1 agonists are incredibly effective medications for the treatment of diabetes and people who are clinically obese. However, “off-label” use has been shown to improve numerous conditions associated with insulin resistance (PCOS), resolve prediabetes, and effectively produce weight loss. For providers who are prescribing these medications, it is important to properly counsel patients to manage their weight loss. Ongoing research, novel triple combination agonist drugs, and oral forms of these powerful weight loss medications offer exciting potential benefits to thousands of patients battling obesity. As with any medication, it is essential to weigh the benefits and potential side effects. Educating patients about potential side effects, including “Ozempic face” will help patients manage distressing changes and allow them to effectively lose weight while maintaining their skin health.
Further reading:
- https://www.americanboardcosmeticsurgery.org/procedure-learning-center/non-surgical/injectable-fillers-guide/
- Blackburn GL, Bistrian BR. Hair loss with rapid weight loss. Arch Dermatol. 1977;113(2):234.
- Kobren SD. Misuse of Ozempic for Rapid Weight Loss Can Cause Significant and Perhaps Permanent Hair Loss. Derm Times. May 14, 2023.
- Busko M. Does Ozempic Cause Hair Loss? Medscape Dermatology. May 25, 2023.
- https://www.medscape.com/viewarticle/992377?form=fpf
- https://www.msn.com/en-us/health/other/what-is-ozempic-face-4-doctors-explain-the-buzzword-and-the-misconceptions-behind-it/ar-BB1pTwCS
- https://www.today.com/health/ozempic-face-rcna67737
- Comparing Ozempic, Wegovy and Other GLP-1 Drugs – GoodRx [Internet]. [cited 2023 Apr 24]. https://www.goodrx.com/classes/glp-1-agonists/glp-1-drugs-comparison
- Tayag Y. Ozempic Is About to Be Old News [Internet]. The Atlantic. 2023 [cited 2023 Apr 22]. Available from: https://www.theatlantic.com/health/archive/2023/04/ozempic-wegovy-mounjaro-weight-loss-drug-development-access/673627/
- LaRose. U.S. Weight Loss Industry Grows to $90 Billion, Fueled by Obesity Drugs Demand. MarketResearch.com
- https://blog.marketresearch.com/u.s.-weight-loss-industry-grows-to-90-billion-fueled-by-obesity-drugs-demand
- Karam, J. Nathan. A Review of FDA-Approved Medications for Chronic Weight Management. Drug Tropics. Aug 5, 2021.
- https://www.drugtopics.com/view/a-review-of-fda-approved-medications-for-chronic-weight-management
- Obesity and overweight. CDC. Updated March 1, 2021. Accessed June 24, 2021. https://ww.cdc.gov/nchs/fastats/obesity-overweight.html