Seasonal Affective Disorder and Your Skin: Understanding the Connection

By Elena Hardy Allbritton, MD
As the temperature drops and the days grow shorter, some people experience a dip in their mood, energy levels, and overall sense of well-being. This phenomenon is commonly referred to as Seasonal Affective Disorder (SAD). While SAD is primarily associated with mood changes, it can also have surprising effects on your skin. In this blog post, we will explore the relationship between Seasonal Affective Disorder and your skin, and offer some healthy ways to combat its effect including some strategies to help you maintain healthy skin during the winter months.
What is Seasonal Affective Disorder (SAD)?
Seasonal Affective Disorder is a form of depression sometimes referred to as “winter depression” because it typically occurs during the fall and winter months when daylight hours are shorter. Women are more commonly affected than men and it typically manifests in younger adults age 18-35. It impacts about 5% of adults or roughly 10 million people in the USA annually.
The decrease in daylight hours is believed to cause a disturbance in the circadian rhythms of the body, which regulates sleep, mood, and other physiological processes. Researchers believe that people with SAD have reduced activity of a brain neurotransmitter called serotonin, which helps regulate mood. Other findings suggest that the overproduction of melatonin, a hormone that is crucial for maintaining normal sleep-wake cycles contributes to the increased sleepiness in patients with SAD. A third factor is lower levels of vitamin D in patients with SAD. Vitamin D and vitamin D responsive elements are found in higher concentrations in the hypothalamus, a region of the brain that contains the circadian rhythm circuitry.
Symptoms of Seasonal Affective Disorder
The most common symptoms of SAD include fatigue, changes in appetite, craving carbohydrate-rich food, weight gain or loss, irritability, difficulty concentrating, and lack of interest in usual activities. However, SAD can also impact your skin in various ways.
Effects of SAD on the Skin:
- Dry Skin: During the winter months, low humidity levels and indoor heating systems can lead to dry, flaky, itchy skin. Individuals with SAD may be more prone to dry skin due to hereditary factors and their ability to retain moisture.
- Eczema and Psoriasis Flares: SAD can trigger or exacerbate some skin conditions such as eczema and psoriasis. Stress, which is often linked to SAD, can weaken the immune system and lead to flare-ups of these conditions which can further worsen the psychosocial impact of SAD. Patients with psoriasis sometimes experience seasonal depression similar to patients with SAD.
- Reduced Collagen Production/Premature Aging: Some Vitamin D is derived from our diets however most vitamin D is produced in the skin when it is exposed to sunlight. Vitamin D is important for the immune system, helps boost serotonin activity, and plays an important role in collagen production. Vitamin D levels in the central nervous system affect the production of serotonin and dopamine, an important neurotransmitter for memory, sense of pleasure/reward, and motivation. Collagen along with Elastin is a key factor responsible for maintaining the skin’s elasticity and preventing premature aging. Individuals with SAD may have lower vitamin D levels which in turn impacts their skin’s overall health and appearance.
- Acne: SAD-induced stress can lead to hormonal imbalances and increased sebum production, which may increase the likelihood of acne breakouts.
Coping Strategies for Healthy Skin for People with SAD:
- Get Adequate Sunlight: Yes, your Dermatologist approves some healthy exposure to natural sunlight, especially for those affected by SAD. While it may be more challenging when the temperatures plummet, try to spend some time outdoors during the daylight hours. Early morning activities in the natural sunlight are preferable to exposure between 10am and 2pm. Even brief exposure such as 20 minutes daily can boost your mood and help your skin get the essential vitamin D that it needs.
- Use Artificial Light Therapy: Using a lightbox to emulate exposure to natural sunlight can alleviate SAD symptoms in just a few days. The gold standard for light therapy is bright white light (color temperature of 5,000 – 10,000 lux). This type of light helps regulate the body’s internal clock. Red LED light therapy, also known as photobiomodulation or low-level laser therapy, has shown promise in the treatment of various conditions, but its role in addressing SAD is still being debated. Red LED light might positively impact people with SAD by having a positive impact on mood and reducing stress. Red light exposure in the evening may help regulate circadian rhythms by influencing melatonin production.
- Moisturize: Combat dry skin with a good-quality moisturizer containing ceramides to repair the lipid barrier of the skin and hyaluronic acid to help retain moisture in the skin. Hyaluronic acid also helps promote collagen production.
- Manage Stress: Stress causes elevated cortisol (“fight-or-flight hormone”) and can weaken the immune system. Finding effective stress management techniques, such as meditation, deep breathing exercises, yoga, hiking outdoors, socializing with others, and talking with a therapist or friend can help reduce the negative impact of stress on your skin.
- Stay Hydrated: Drinking adequate water is crucial for maintaining overall skin health. Hydration from the inside out can help fight dryness and keep the skin more supple.
- Eat a Balanced Nutrient-Rich Diet: Vitamins A, C, and D are important for collagen production. Foods rich in antioxidants (berries, citrus fruits, and broccoli) and tryptophan (turkey, bananas) can help alleviate some symptoms.
- Use Sunscreen: Even on cloudy winter days, UV rays can still harm your skin. Protect yourself when spending time outdoors by applying sunscreen with at least SPF 30. Mineral sunscreens containing zinc or titanium oxide offer more broad spectrum protection against damaging UVA and UVB rays.
- Seek Professional Help: If your skin conditions worsen during the winter months and it is affecting your quality of life, consult your dermatologist. We can provide targeted advice, customized skin regimens, and treatments for your skin issues.

Grassroots Health Nutrient Research Institute
Conclusion
Seasonal Affective Disorder can have a surprising impact on your skin, from dryness and eczema flare-ups to reduced collagen production and premature aging. To combat these effects, it is important to take steps to care for your skin and your overall wellness during the winter months.
By managing stress, maintaining good skincare habits, and seeking professional help when necessary, you can keep your skin healthy and radiant even in the darkest of seasons. Some people may find that changing geographical locations to be closer to the equator is necessary, however, most people can find relief by adopting certain changes. Remember that your skin is not just an external reflection of your health; it can also be an indicator of your emotional well-being.
Resources for Further Reading
American Academy of Dermatology: https://www.aad.org/
National Institute of Mental Health – Seasonal Affective Disorder: https://www.nimh.nih.gov/health/topics/seasonal-affective-disorder/index.shtml
Sources
12 notable seasonal Affective disorder statistics. HRF. September 4, 2014. Accessed October 30, 2023. https://healthresearchfunding.org/seasonal-affective-disorder-statistics/.
Seasonal affective disorder: Symptoms, causes, diagnosis and treatments. Msn.com. Accessed October 29, 2023. https://www.msn.com/en-us/health/condition/Seasonal-affective-disorder/hp-Seasonal-affective-disorder?source=conditioncdx.
Seasonal Affective Disorder. National Institute of Mental Health. NIH Publication No. 20-MH-8138. https://www.nimh.nih.gov/health/publications/seasonal-affective-disorder.
Stewart, Alan E et al. “Possible contributions of skin pigmentation and vitamin D in a polyfactorial model of seasonal affective disorder.” Medical hypotheses vol. 83,5 (2014): 517-25. doi:10.1016/j.mehy.2014.09.010
Seasonal affective disorder. Mayo Clinic. December 14 2021. https://www.mayoclinic.org/diseases-conditions/seasonal-affective-disorder/symptoms-causes/syc-20364651
How is vitamin D made by the sun different from vitamin D in supplements? Grassroots Health Nutrient Research Institute. May 8 2023. https://www.grassrootshealth.net/blog/vitamin-d-made-sun-different-vitamin-d-supplements/




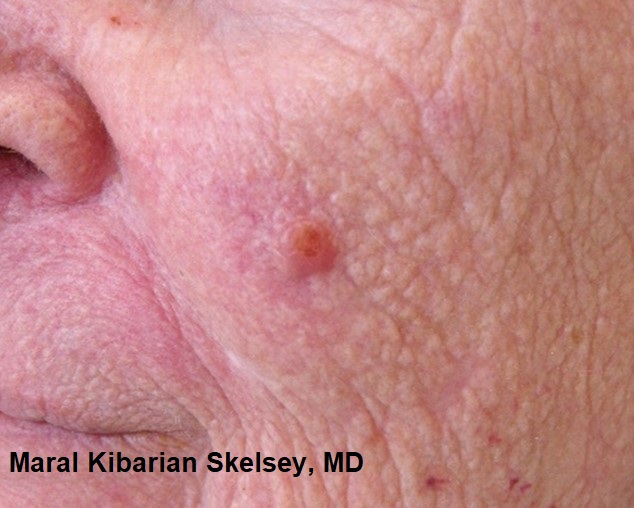 What does this skin cancer look like?
What does this skin cancer look like?