Skin Cancer Myths
By Caroline Glick, PA-C, MPH
In the United States, skin cancer is the most common type of cancer. One in five Americans will develop skin cancer in their lifetime. Despite such high numbers of skin cancer diagnoses, there are many myths pertaining to skin cancer and sun protection. In this post, I will debunk some of these common myths.
Common Skin Cancer Myths
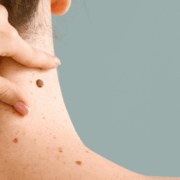
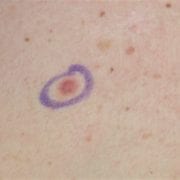
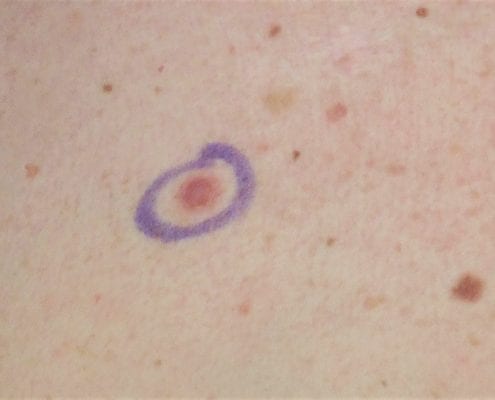
MYTH: Skin cancer always looks like a dark spot.
FACT: Skin cancer can have many different appearances. Skin cancer can sometimes look like a pink patch of skin, a pearl-like bump, a scaly patch, a bleeding bump, or a sore that will not heal. Sometimes, skin cancer can also be a dark, raised, or irregular spot. If you notice any of these changes on your skin, please make an appointment to see us.

MYTH: Melanoma is the only type of skin cancer.
FACT: There are multiple types of skin cancers. The most prevalent types of skin cancers are basal cell carcinoma, squamous cell carcinoma, and melanoma. Basal cell carcinoma is the most common type of skin cancer. Melanoma is the most serious type of skin cancer. In the United States, it is estimated that melanoma will cause more than 8,400 deaths in 2025.
MYTH: Skin cancer is not treatable.
FACT: If caught early, most skin cancers can be highly curable. In fact, patients diagnosed with melanoma who are treated before the melanoma spreads to the lymph nodes have a five-year survival rate of 99%. Regular skin checks at a dermatology practice are important for early detection and treatment of skin cancers.
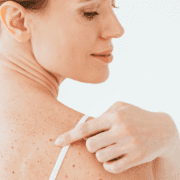
MYTH: Skin cancer can only occur on sun-exposed areas.
FACT: Skin cancer can occur anywhere on the skin. It can occur under the nails, on the palms of the hands, on the soles of the feet, and on the genitalia. However, the most common areas where skin cancer can develop are on sun-exposed locations, including the scalp, face, ears, neck, chest, arms, and legs.
MYTH: Skin cancer only occurs in older people.
FACT: Among adolescents and young adults aged 15-29 years old, melanoma is the second most commonly diagnosed cancer. Men aged 49 years old and under are more likely to develop melanoma than any other cancer, except for colon and rectal cancers. Women aged 49 years old and under have a higher probability of developing melanoma than any other type of cancer, except breast and thyroid cancers. It is important to have regular skin examinations at a dermatology practice so skin cancers can be detected and treated early.
MYTH: Make-up provides adequate sun protection.
FACT: Some make-up does contain sunscreen, but make-up usually does not provide enough protection from the harmful Ultraviolet (UV) rays of the sun. Sunscreens should be broad-spectrum with coverage against both UV-A and UV-B and at least SPF 30. Sunscreen also needs to be applied multiple times a day for it to be effective. In fact, sunscreen should be applied every two hours, even if the sunscreen is a high SPF.
MYTH: Sunscreens never expire.
FACT: According to the Food and Drug Administration (FDA), sunscreens lose their efficacy and are not as strong after three years. Please always check the bottle for the expiration date and replace sunscreens as needed.
MYTH: It is only necessary to wear sunscreen on sunny, hot days at the beach.
FACT: Sunscreen should be worn every day, even on cloudy and cold winter days.
Clouds can reduce UV rays by only 50%. The remaining UV can still cause sun damage to the skin. And remember to apply sunscreen when at high altitudes, for example, when hiking or skiing. UV increases by 6% for every 1000 feet of elevation gain. When skiing, snow reflects UV rays.
MYTH: Tanning beds are safer than tanning at the beach.
FACT: There is no such thing as safe tanning, whether it is at the beach or a tanning salon. Using a tanning bed before the age of 35 can increase the risk of melanoma by 75%. Also, getting a base tan does not prevent sunburn. All tanning causes DNA damage in the skin, which increases the risk of getting skin cancer.
These myths are just some of the misconceptions about skin cancer. With summer right around the corner and more time spent outdoors, it is important to remember that early detection is key to treating skin cancer. If you notice any changes on your skin that do not resolve within six weeks, please make an appointment with one of the providers at the Dermatologic Surgery Center of Washington. Have a wonderful summer and remember your hats and sunscreen!
Resources
10 Skin Cancer Myths Debunked. University of Texas MD Anderson Cancer Center. Accessed April 14, 2025. Retrieved from https://www.mdanderson.org/publications/focused-on-health/10-skin-cancer-myths-debunked.h14-1592991.html.
10 Surprising Facts About Indoor Tanning. American Academy of Dermatology. April 26, 2023. Accessed April 14, 2025. Retrieved from https://www.aad.org/public/diseases/skin-cancer/surprising-facts-about-indoor-tanning.
May is Skin Cancer Awareness Month. American Academy of Dermatology. April 13, 2024. Accessed April 14, 2025. Retrieved from https://www.aad.org/public/public-health/awareness-campaigns/skin-cancer-awareness-month.
Skin Cancer Facts and Statistics. Skin Cancer Foundation. February 2024. Accessed April 16, 2025. Retrieved from https://www.skincancer.org/skin-cancer-information/skin-cancer-facts/.
Skin Cancer. American Academy of Dermatology. February 25, 2025. Accessed April 14, 2025. Retrieved from https://www.aad.org/media/stats-skin-cancer.
The Most Common Misconceptions About Skin Cancer. American Society for Mohs Surgery. February 15, 2024. Accessed April 14, 2025. Retrieved from https://www.mohssurgery.org/blog/skin-cancer/the-most-common-misconceptions-about-skin-cancer/
Top 5 Myths About Sunscreens. Mayo Clinic. May 26, 2023. Accessed April 14, 2025. Retrieved from https://www.mayoclinichealthsystem.org/hometown-health/speaking-of-health/myth-or-fact-coconut-is-an-effective-sunscreen
Weir, H. K., Marrett, L. D., Cokkinides, V., Barnholtz-Sloan, J., Patel, P., Tai, E., Jemal, A., Li, J., Kim, J., & Ekwueme, D. U. (2011). Melanoma in adolescents and young adults (ages 15-39 years): United States, 1999-2006. Journal of the American Academy of Dermatology, 65(5 Suppl 1), S38–S49. https://doi.org/10.1016/j.jaad.2011.04.038