Measles: What it is and How to Prevent it
With cases in the United States on the rise, many are seeking more information about the measles virus and how it could impact them. Measles is a viral respiratory illness that can cause serious complications. Worldwide, measles causes 1 million deaths per year in children under 5 years old. In 2024, there were a total of 285 cases in the United States. As of March 25, 2025, there have been 378 reported cases: two in Prince George’s County and one in Howard County.3,5 Ninety-five percent of those infected were unvaccinated. To date, there have been 2 deaths associated with measles in the United States in 2025.3 With the uptick of cases seen this year, it is important to be aware of how we can mitigate the infection.
How Measles is Spread
The measles virus is highly contagious and spreads either through direct contact or via airborne particles that are spread when an infected individual sneezes, coughs, or talks. The measles virus can remain infectious in the air for up to 2 hours after the infected person leaves the area, whether or not the patient was masked. Patients with measles should remain in airborne precautions for 4 days after the onset of their rash.
What does Measles look like?
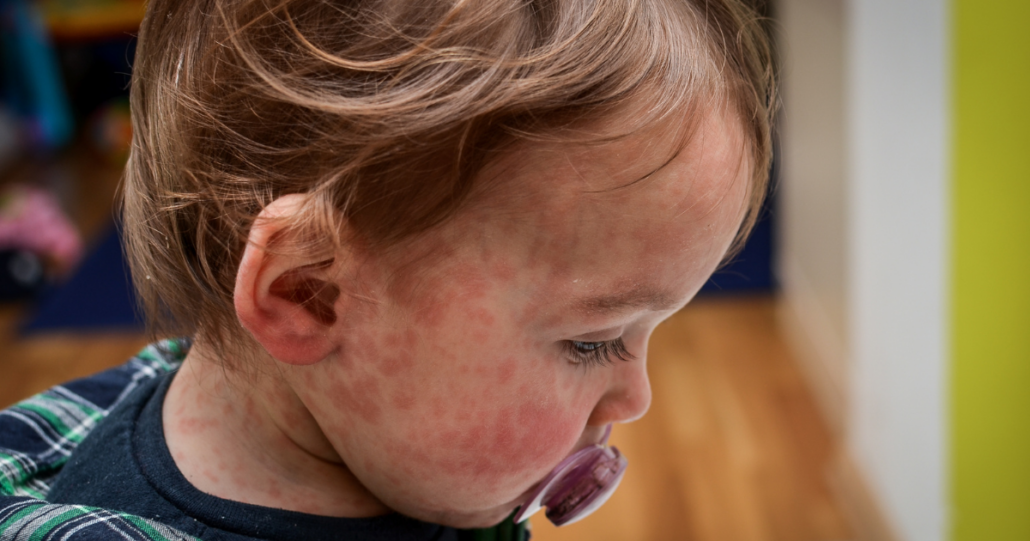
Measles often begins with a prodrome, or early symptoms, that precede the rash and begin an average of 10-12 days after exposure. The characteristic prodrome consists of fever, malaise, and the 3 C’s: cough, coryza (runny or stuffy nose), and conjunctivitis. During this period, you may also begin to notice white spots inside the mouth, called Koplik’s spots, that are highly indicative of a measles infection. This prodrome typically lasts about 2 to 4 days. Following about 14 days after exposure, a non–itchy rash consisting of red spots develops. This rash typically appears first on the head, most often behind the ears, then progresses to involve the rest of the body, spreading from the head to the toes, and often sparing the palms of the hands and the soles of the feet. This rash typically subsides after about 1 week of fever resolution. Infected individuals are contagious for approximately 4 days before the onset of the rash and 4 days after the rash appears.
Measles infection can lead to various complications, including ear infections, diarrhea, or pneumonia, with pneumonia the most common cause of measles-related death. Rarely, measles can lead to encephalitis, or inflammation of the brain, occurring in about ~0.1% of children. This can lead to permanent brain damage, and may become potentially fatal in 10-20% of patients. Of the reported cases of measles, ~30% of individuals experience one or more complications.2
Women exposed to measles during pregnancy have an increased risk of complications, including increased risk of premature labor, miscarriage, and low birthweight.
Preventing the Spread of Measles
The only way to prevent measles infection is through vaccination. There is no antiviral medication. The MMR vaccine, which vaccinates against Measles, Mumps, and Rubella, is recommended at ages 12-15 months and 4-6 years old. One dose of the MMR vaccine is 93% effective against measles infection, with prevention increasing to 97% with the second dose.
Prior to the implementation of the MMR vaccine, there were approximately 3-4 million measles cases in the United States each year, accounting for 400-500 deaths. Following the introduction of the vaccine, the yearly cases dropped significantly, with only 37 yearly cases reported by 2004.1
When 95% of the community is vaccinated against measles, we reach herd immunity, a phenomenon in which a sufficient portion of the population becomes immune to a disease, thereby reducing its spread and providing indirect protection to individuals who are not immune.
Currently in the United States, we are below the threshold required for herd immunity with 92.7% of kindergarten-aged children being vaccinated, increasing the risk of infection for those without immunity.3
As the MMR is a live, attenuated vaccine, it may be contraindicated in certain immunocompromised populations, making the need for herd immunity even more important for those who cannot receive the vaccine but are at risk.
International travel has been a leading cause of measles infection in the United States. The CDC recommends getting the vaccine at least 2 weeks before departure, with one dose recommended for infants aged 6-11 months and 2 for those 12 months and over.
What to do if you have Measles
If you think you or your child may be infected with measles, call your primary care provider or urgent care facility and tell them you suspect measles. Do not proceed without calling ahead. You may be directed to a facility with an airborne infection isolation room (AIIR); the facility will provide you with specific instructions, including entering through a separate entrance to prevent the risk of spreading to other patients and healthcare workers. The patient and accompanying family members should wear a mask or should be “tented” if masking is not tolerated.
As cases of measles continue to rise in the United States, with new confirmed cases in Maryland, it is essential we work to counteract its spread through vaccination. If you are unable to find your vaccination records or have specific questions about vaccination recommendations, talk to your primary care physician.
Resources
- Gastanaduy P, Haber P, Rota P, Patel M. Chapter 13: Measles. Centers for Disease Control and Prevention. April 24, 2024. Accessed March 13, 2025. https://www.cdc.gov/pinkbook/hcp/table-of-contents/chapter-13-measles.html.
- James WD, Elston DM, Treat J, Rosenbach M, Neuhaus IM, Andrews GC. Measles. In: Andrews’ Diseases of The Skin: Clinical Dermatology. Elsevier; 2025.
- Measles cases and outbreaks. Centers for Disease Control and Prevention. March 7, 2025. Accessed March 12, 2025. https://www.cdc.gov/measles/data-research/index.html#cdc_data_surveillance_section_1-measles-cases-in-2024.
- Marks JG, Miller JJ, Lookingbill DP. Measles. In: Lookingbill and Marks’ Principles of Dermatology. Saunders Elsevier; 2019.
- Maryland Department of Health Center for Immunization. Maryland.gov Enterprise Agency Template. Accessed March 25, 2025. https://health.maryland.gov/phpa/OIDEOR/IMMUN/Pages/Measles.aspx.
- History and current status. American Academy of Dermatology. Accessed March 25, 2025. https://www.aad.org/member/clinical-quality/clinical-care/emerging-diseases/measles/history-current-status.





